The Reason Our Skin Itches Is Grosser Than You Think
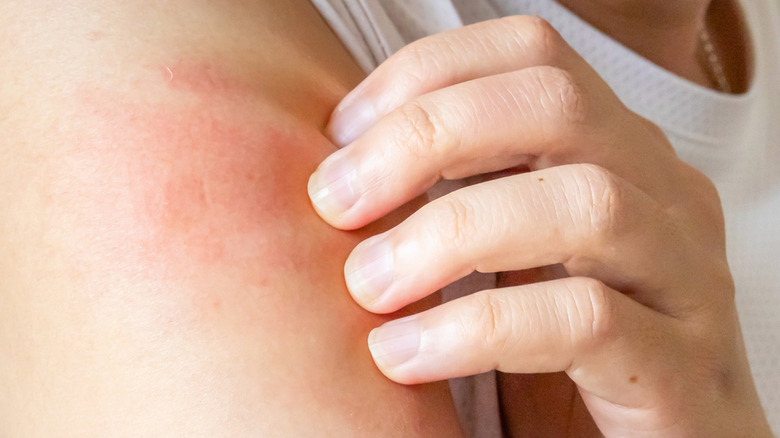
When you have itchy skin, you might attribute it to just dry skin, hives, insect bites, or a condition like eczema or psoriasis. It could even be an allergic reaction or irritation caused by a chemical, soap, or wool. However, there's a more disgusting reason that your skin could start itching: Staphylococcus aureus, which is responsible for a variety of bacterial infections in humans.
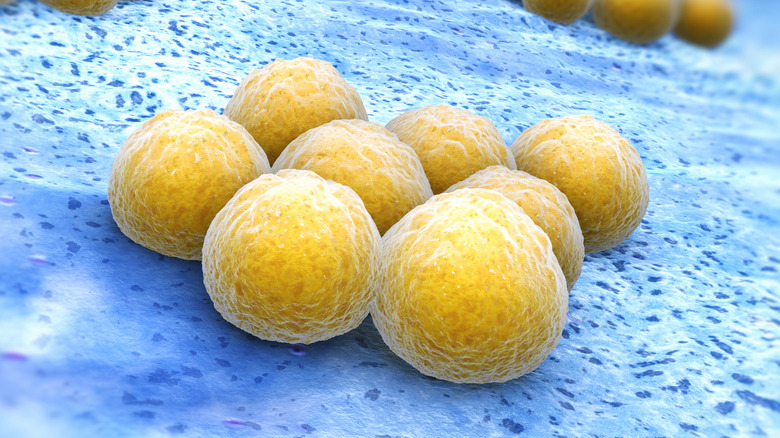
According to research performed in Harvard Medical School's Chiu Lab and published in Cell, S. aureus can trigger itchy skin by directly activating sensory nerves in the epidermis (the outermost skin layer). This bacterial pathogen falls into one of three main categories of bacteria known as coccus bacteria. The new studies on mice and human cells indicate that, when the balance of the healthy microorganisms in the skin is disrupted, S. aureus can flourish. Upon contact, the bacteria emit an enzyme called protease V8 that sparks activity in the protein PAR1 on the epidermal nerve fibers. That V8 provokes a molecular chain reaction that sends signals to the brain, resulting in the itch-and-scratch cycle.
After exposing mice to S. aureus, the researchers witnessed the animals develop an itch that intensified for several days, and worsening skin damage spread beyond the exposure point with constant scratching. One of the study's authors, Isaac Chiu said in a statement, "We've identified an entirely novel mechanism behind itch — the bacterium Staph aureus, which is found on almost every patient with the chronic condition atopic dermatitis. We show that itch can be caused by the microbe itself."
What discovering S. aureus as an itch trigger means
Finding out that Staphylococcus aureus releases a chemical that activates the PAR1 protein to send itch signals to the brain was just one part of the research. Along with witnessing the heightened itch during experiments on mice, the researchers were also able to treat the itch. Since PAR1 has a role in blood-clotting, they tried treating the S. aureus–infected mice with an anticlotting medication that blocks the protein. The mice experienced rapid improvement, and as a result, the scientists recorded a dramatically reduced need to scratch and less scratching-related damage to the skin — the largest organ in the body.
Because of the results of this research, it's possible that the medical community could repurpose the PAR1-blocking medication as an anti-itch medication. They could even isolate the active ingredient to use as the base of a topical cream. In particular, this treatment could be used for inflammatory skin conditions, such as atopic dermatitis (chronic eczema). They arrived at this theory because, when comparing atopic dermatitis skin samples from humans to healthy samples, they found higher levels of S. aureus and V8 in those infected samples.
Beyond that, this research raises the question as to why S. aureus causes itchy skin. It's possible that the release of V8 and hijacking of epidermal nerve fibers benefits the bacteria. Co-author Liwen Deng said in a statement, "It's a speculation at this point, but the itch-scratch cycle could benefit the microbes and enable their spread to distant body sites and to uninfected hosts." Follow-up studies could pinpoint the answer and determine whether or not other bacteria cause itch.